How ADHD Affects Teen Health In 2026: What The CDC Data Actually Tells Parents
ADHD changes how teenagers sleep, use screens, make friends, and handle daily stress. A 2025 CDC study published in the Journal of Developmental & Behavioral Pediatrics confirms this with something most prior research lacked: the teens' own words. Researchers collected self-reported data from 12- to 17-year-olds across the U.S. between July 2021 and December 2022, and the results challenge several assumptions parents and clinicians have operated on for years.
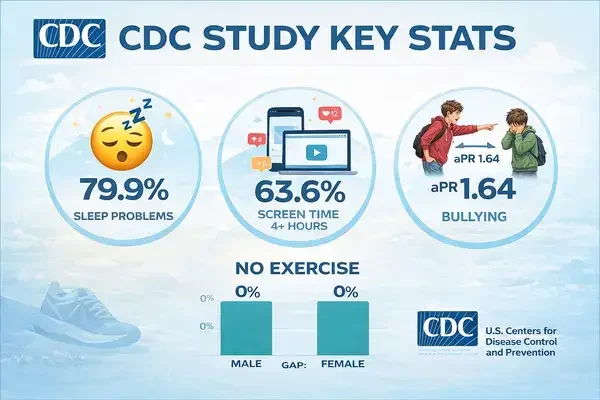
ADHD affects roughly 10.4% of U.S. teenagers, according to 2025 CDC data. Teens with ADHD report higher rates of bullying, more sleep problems, and more daily screen time than their peers. They don't, however, show lower physical activity levels, which contradicts older research focused on younger children.
I've worked in content strategy across health and education verticals for over a decade, and this study stands out for one reason: it asked teens directly instead of relying on parent or clinician reports. That distinction matters more than most people realize. Parents often underestimate bullying and overestimate how much sleep their kids are getting. When you skip the teen's perspective, you get a half-finished picture.
This article breaks down what the CDC found, where it conflicts with older data, and what parents and executive function coaches should do with these numbers. We won't cover medication management or formal diagnosis criteria here. Those deserve their own space, and plenty of other resources handle them well.
What Does the 2025 CDC Teen Self-Report Study Actually Say?
The study (Katz et al., 2025) pulled data from the National Health Interview Survey's teen module, covering a nationally representative sample. About 10.4% of teens in the sample had a parent-reported ADHD diagnosis. But the health behavior data came from the teens themselves.
That's the part that matters. Previous national datasets on teen ADHD relied almost entirely on what parents told researchers. CHADD (Children and Adults with Attention-Deficit/Hyperactivity Disorder), the leading national ADHD nonprofit and a CDC partner, emphasized this point in their 2025 conference coverage: direct teen input reveals gaps that parent-only reports consistently miss.
The researchers compared adjusted prevalence ratios (aPR) between teens with and without ADHD across several categories. The biggest gaps showed up in sleep, screen time, and social experiences. Physical activity, which many clinicians expected to be lower in teens with ADHD, showed no statistically significant difference.
Actually, that last finding deserves more attention than it's gotten. I'll come back to it.
Why Do Teens With ADHD Get Bullied More But Still Report Peer Support?
Teens with ADHD reported bullying at a rate 64% higher than their peers (aPR 1.64). They also reported 83% more difficulty making friends (aPR 1.83). Those numbers are severe.
But here's the contradiction that most coverage of this study breezes past: teens with ADHD were less likely to report a lack of peer support (aPR 0.70). They're getting bullied more, struggling to make friends, yet they don't feel unsupported.
A few possible explanations. One is that teens with ADHD may form fewer but more intense friendships. Another is that their self-perception of support doesn't match what clinicians or parents would consider adequate support. And a third, which I've seen play out with families I've talked to through our work: these teens often rely heavily on one or two close relationships, which feel like "enough" even when the broader social picture is rough.
The Child Mind Institute notes that about half of adolescents with ADHD have serious problems with peer relationships, and they're more likely to be ignored, rejected, or bullied. But impaired social skills don't mean zero social connection. The distinction matters because interventions that focus only on building new friendships may miss the real need, which is protecting and strengthening the relationships these teens already have.
Schools rarely ask teens directly about their social experience. They rely on teacher observations or parent reports. This study makes a strong case for changing that, and it's something families working with ADHD coaches should push for during IEP and 504 meetings.
How Bad Is the Sleep Problem for Teens With ADHD?
Bad. About 79.9% of teens with ADHD reported sleep problems, compared to 69.1% of teens without. That gap might look modest at first glance, but the specific sleep issues tell a rougher story.
Irregular wake times were more than twice as common in teens with ADHD (aPR 2.17). Difficulty getting out of bed was 29% more likely (aPR 1.29). These aren't teens who just "stay up too late." Their circadian rhythm regulation is disrupted at a biological level, and the downstream effects hit everything: attention during school, emotional control, and the ability to start tasks on time.
I've seen a pattern across dozens of families: parents treat the morning chaos as a behavior problem instead of a sleep architecture problem. They set earlier bedtimes, take away phones at night, and still end up dragging their kid out of bed. That's because the issue isn't just when teens with ADHD sleep. It's how their brains cycle through sleep stages.
Research from Nature (January 2026) reinforces this. Light from screens suppresses melatonin production, and that effect is most pronounced in adolescents. For a teen with ADHD who already has impaired sleep regulation, the combination of screen exposure and biological vulnerability creates a feedback loop that earlier bedtimes alone won't fix.
Practical takeaway: if your teen with ADHD can't wake up, don't start with discipline. Start with a sleep assessment. Talk to your pediatrician about melatonin timing, light exposure, and whether a formal sleep study is warranted. And if you're working with a coach on building better morning routines, make sure they understand the biological component. Without that foundation, every routine you build will collapse by Thursday.
Does Screen Time Make ADHD Worse in Teenagers?
The CDC study found that 63.6% of teens with ADHD spend four or more hours per day on screens (excluding schoolwork), compared to roughly half of teens without ADHD (aPR 1.26). That's a lot of non-academic screen time.
But here's where most ADHD content gets it wrong. They frame this as "ADHD kids are addicted to screens." The reality is more complicated. A 2023 longitudinal study of nearly 4,000 Canadian high school students (published in Scientific Reports) found that impulsivity mediates the relationship between screen time and ADHD symptoms. Social media, specifically, showed a lagged within-person association with worsening symptoms. It's not that screens cause ADHD. It's that the ADHD brain's reward system makes screens harder to put down, and the extended use then makes symptoms worse.
Nature reported in January 2026 that adolescents with ADHD are disproportionately likely to use social media in risky ways: sharing personal information, staying online past midnight, and engaging in interactions that damage real-world friendships. The feedback loop goes both directions.
The contrarian take I'll offer: blanket screen time limits ("two hours max!") don't work well for teens with ADHD because they don't address why the teen is on screens. A teen scrolling TikTok for dopamine hits needs a different intervention than a teen using Discord to maintain their only stable friendship. One-size-fits-all rules treat the symptom and ignore the function.
Families should track what their teen does on screens, not just how long. Then work with a professional who understands the connection between ADHD and screen habits to build a plan that replaces screen time with activities that meet the same underlying need.
What About Physical Activity? The Surprising Finding
Most parents and even some clinicians assume teens with ADHD are less active. Older studies on younger children supported that assumption. But the 2025 CDC data says otherwise.
There was no statistically significant difference in physical activity levels between teens with and without ADHD. About 75.5% of teens with ADHD got fewer than 60 minutes of daily activity, compared to 74.3% of teens without ADHD. Functionally identical.
This is good news with a caveat. It doesn't mean exercise is irrelevant for teens with ADHD. A 2026 study in Humanities and Social Sciences Communications analyzed data from over 50,000 U.S. children and found that physical activity was the strongest mediator between screen time and mental health problems, accounting for 30.9% to 38.9% of the association. For teens with ADHD who are already at risk from high screen time and poor sleep, exercise may be the single most protective daily behavior.
The finding also suggests that earlier studies conflated childhood ADHD activity levels with adolescent ones. Kids with hyperactive-type ADHD may actually be more active than peers in elementary school, then normalize in the teen years as hyperactivity symptoms shift toward internal restlessness. The data matches what research on ADHD symptom changes across ages has been suggesting for years.
What Should Parents and Schools Do Differently in 2026?
The study's authors recommend health promotion programs designed specifically for teens with ADHD. That's a polite way of saying "stop using the same playbook you use for neurotypical teens." Fair enough. But what does that look like in practice?
Ask teens directly. This is the study's loudest message. Parent reports miss things. Teacher reports miss things. The teen is the only person who knows if they're being bullied at lunch, staring at their ceiling until 2 AM, or doom-scrolling when they should be studying. Build check-ins into coaching sessions, therapy appointments, and IEP reviews that give the teen space to report their own experience.
Treat sleep as a medical issue, not a discipline issue. When 80% of teens with ADHD report sleep problems and irregular wake times are twice as common, you're not dealing with laziness. You're dealing with circadian disruption. Bring it up with your pediatrician. Consider a referral to a sleep specialist. Adjust school-morning expectations accordingly.
Get specific about screen time. "Less screen time" is too vague. Track what platforms your teen uses, when they use them, and what purpose the usage serves. Then set boundaries that address the specific risks (late-night social media, passive scrolling) while preserving the screen activities that actually serve a social or educational function.
Don't ignore social skills just because your teen has friends. The CDC data shows teens with ADHD can feel supported while still experiencing high rates of bullying and social difficulty. Having a friend group doesn't mean the social picture is healthy. Schools should follow CDC classroom guidance for ADHD and screen for bullying among ADHD students directly, not wait for a parent or teacher to notice.
Protect physical activity. The fact that teens with ADHD aren't less active is a positive finding. Keep it that way. Don't pull them from sports or extracurriculars as a consequence for academic struggles. Exercise may be the most effective buffer against the sleep and screen time problems this study documents.
Parents who feel overwhelmed by this list aren't wrong to. It's a lot. Working with a team that specializes in ADHD support or connecting with an organization like CHADD can help you prioritize and build a realistic plan. The worst thing you can do is try to fix everything at once. Pick the area where your teen struggles most (for most families, that's sleep or screens) and start there.
Are ADHD Diagnosis Rates Still Rising in Teens?
Yes. CDC data updated in November 2024 shows that 11.4% of U.S. children aged 3 to 17 (roughly 7 million) have received an ADHD diagnosis at some point. That's up from approximately 9.4% a decade ago. The increase reflects better recognition of ADHD in girls and greater diagnostic access post-pandemic, according to CHADD's analysis of the data.
Among those with current ADHD, 77.9% have at least one co-occurring condition (anxiety, depression, learning disorders, behavioral issues). Only 53.6% received medication in the past year, and just 44.4% got behavioral treatment. That means 30.1% of kids with a current ADHD diagnosis received no ADHD-specific treatment at all.
That last stat should bother everyone. Three out of ten diagnosed kids getting zero treatment isn't a gap. It's a failure. And for teens specifically, the consequences compound fast: missed academic milestones, damaged social relationships, and sleep problems that carry into adulthood.
NCHS demographic data and CHADD both note that state-level diagnosis rates range from 6% to 16%, driven largely by differences in insurance access and provider availability. If you're in a state with lower diagnosis rates, it may not mean fewer kids have ADHD. It may just mean fewer kids are getting identified.
FAQs
How does ADHD affect teen sleep according to the latest research?
The 2025 CDC study found that 79.9% of teens with ADHD report sleep problems, compared to 69.1% of teens without. Irregular wake times are more than twice as common (aPR 2.17), and difficulty getting out of bed is 29% more likely. These patterns point to circadian rhythm disruption, not just poor sleep habits.
Why are teens with ADHD bullied more often?
Teens with ADHD reported 64% higher rates of bullying (aPR 1.64) and 83% more difficulty making friends (aPR 1.83) in the CDC study. Impaired social cues, impulsive behavior, and emotional reactivity can make them targets. The Child Mind Institute reports that about half of adolescents with ADHD have serious peer relationship problems.
How much screen time do teens with ADHD typically have?
About 63.6% of teens with ADHD spend four or more hours daily on non-school screens (aPR 1.26 compared to peers without ADHD). Research suggests impulsivity mediates this relationship, meaning the ADHD brain's reward-seeking patterns make it harder to disengage from screens.
Does ADHD make teenagers less physically active?
No, according to the 2025 CDC data. About 75.5% of teens with ADHD and 74.3% without ADHD got fewer than 60 minutes of daily physical activity. There was no statistically significant difference, which contradicts older studies focused on younger children with ADHD.
What percentage of teens are diagnosed with ADHD in the United States?
Approximately 10.4% of U.S. teens aged 12 to 17 have a parent-reported ADHD diagnosis, according to 2021–2022 CDC data. The broader childhood figure (ages 3 to 17) is 11.4%, reflecting roughly 7 million children as of the 2024 update.
How does ADHD affect teen health differently than childhood ADHD?
Teen ADHD tends to shift away from visible hyperactivity toward internal restlessness, executive function struggles, sleep disruption, and social-emotional challenges. The 2025 CDC study is the first national dataset to capture these patterns through teen self-reports rather than parent or clinician observations alone.
What should parents do if their teen with ADHD can't wake up in the morning?
Start with a medical evaluation rather than stricter rules. The CDC data shows irregular wake times are 2.17 times more common in teens with ADHD. Discuss melatonin timing and light exposure with a pediatrician. Consider a referral to a sleep specialist. Behavioral strategies work best when layered on top of proper sleep support, not as a replacement for it.